AI in SNF Reimbursement: The Gap No One Is Talking About
AI in SNF reimbursement is everywhere in healthcare right now. For leaders responsible for reimbursement in skilled nursing, the real question is simple: does it actually change how teams operate?
Reimbursement has become one of the most complex challenges in skilled nursing. Organizations must simultaneously manage Medicare PDPM, state-specific Medicaid case mix systems, a growing number of Medicare Advantage contracts, and Quality Incentive Programs. Each payer has its own requirements, timelines, and financial implications, creating a system that is not just complex, but constantly shifting.
What makes this even more challenging is that reimbursement is not stagnant. It evolves across the entire resident stay. Clinical conditions change, documentation builds across disciplines, and each payer type influences outcomes in ways that are not always immediately visible.
Over the past several years, different categories of technology have emerged to help. Solutions in this space range from admissions optimization to MDS completion support and auditing tools that look for reimbursement keywords in documentation.
While these approaches address important parts of the reimbursement process, they are largely tied to specific workflow moments and depend on retrospective or manual interpretation of what has already happened.
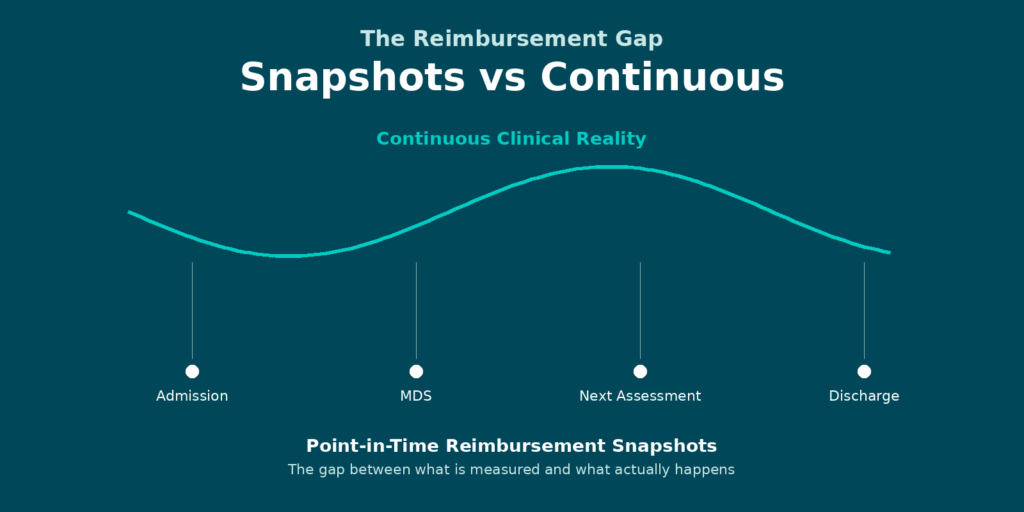
And that is where the gap becomes impossible to ignore.
Clinical and functional changes occur continuously, not just during assessments. In a world where every Medicare Advantage plan may interpret level of care differently, and where Medicaid and quality programs require early awareness, missing those details has real financial and operational consequences.
Historically, teams have relied on manual review to bridge this gap. That approach is no longer sustainable. The volume, variability, and speed of change have outpaced what even the strongest teams can manage consistently.
The next phase of AI in skilled nursing is not about improving isolated tasks. It is about creating continuous visibility across the entire reimbursement lifecycle, with the ability to manage change in the context of each payer’s requirements.
Organizations that have moved in this direction are seeing measurable results, including improved case mix, stronger Medicare alignment, and better performance across Medicare Advantage and quality programs. Just as importantly, they are seeing a shift in how their teams operate, with less time spent searching for issues and more time focused on action.
That shift becomes particularly clear in complex, multi-state organizations where variability across payers is not theoretical, but a daily operational reality. As Lisa Sinatra, Senior Director of Clinical Reimbursement at Ciena Healthcare, explains:
“When you operate across multiple states and across all payers, reimbursement complexity is a given. Every state has nuances, and Medicare, Medicaid, and Managed Care all have their own expectations. MedaSync brings clarity to payer complexity and gives us confidence that nothing is slipping through the cracks.”
More importantly, that visibility changes how teams operate day to day. Instead of relying on retrospective reports or time-intensive chart reviews, leaders are able to see where performance is shifting as it happens and respond before issues escalate.
“What really stands out is how MedaSync helps us stay proactive. We are not waiting for problems to show up on a report weeks later. MedaSync gives us the visibility to see trends early, support our teams in real time, and protect performance before issues escalate.”
As reimbursement complexity continues to grow, the ability to see clearly across all payers, including the nuances of individual Medicare Advantage contracts, will become increasingly critical. AI has a role to play, but only when it is applied in a way that reflects the reality of how reimbursement actually works.
In a system defined by constant change, visibility is no longer optional. It is the difference between reacting to performance and actually managing it.
See What You Might Be Missing Across Your Payer Mix
If you are rethinking how reimbursement is managed across Medicare, Medicaid, Medicare Advantage, and quality programs, it may be time to look more closely at what continuous visibility could uncover.





